As a follow on from last month’s article discussing Jumper’s Knee (Patella Tendonitis) this month’s article covers another chronic injury that can blight the rugby knee.
Iliotibial Band Friction Syndrome (“ITBFS”)
As its common name suggests, this condition is found in runners (but can also affect cyclists). ITBFS is often referred to as an overuse injury causing pain to the outer part of the knee. However, there are other issues that can make an athlete more susceptible, particularly weak gluteus medius, tight or wide iliotibial band (“ITB”), trigger points in both areas and fallen arches (over pronation).
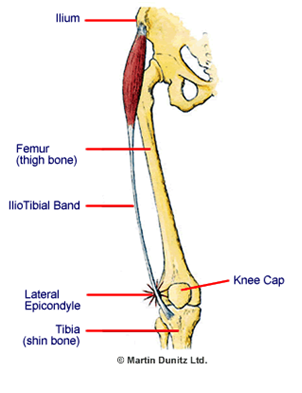
As you can see from the front-on illustration, the ITB is a superficial sheet of fascia with vertical fibres running along the outside of the thigh, connecting the hip and the knee. It is responsible for flexing, medially rotating and abducting the hip.
As the knee bends and straightens the distal ITB moves from in front to behind and back in front of the lateral epicondyle, the small bony prominence at the lower end of the femur (thigh bone) on the outside of the knee.
When this movement is repeated, as in running, this can cause friction, which more often than not leads to inflammation of the surrounding soft tissue.
- Symptoms:
- Pain on the outside of the knee, which can radiate upwards or downwards;
- Tightness along the outside of the thigh;
- Pain becomes worse when running;
- Pain when bending and straightening the knee, which intensifies when the area is pressed; and
- Weakness in hip abduction.
Although ITBFS can be diagnosed with an MRI scan, it will not be evident with an x-ray.
Treatment
Rest and cold therapy will help to reduce inflammation and pain but if ITBFS is diagnosed the first port of call should be postural assessment and biomechanical analysis to eliminate issues in this area.
Sessions with a L4/5 Sport and Remedial Massage Therapist (“SRMT”) will help to eliminate trigger points whilst softening the ITB and surrounding tissues appropriately. If weakness is found in the gluteus medius, a therapist will also be able to help strengthen this area.
If the above treatment is unsuccessful, referral for a corticosteroid injection may be considered.
Prevention
My most preferred prevention method (as a prehabilitator) is to eliminate all the associated issues prior to activity. As always, make sure your posture and mechanics are good.
Spend time during your off season strengthening the areas surrounding the ITB, paying particular attention to the gluteus medius.
Stretching the ITB is a matter of contention as the ITB is not actually a muscle. There are many ‘ITB stretches’ recommended such as the one below but these only ‘appear’ to stretch the ITB. They actually stretch the Tensor Fascia Latae; the muscle you can see at the top of the ITB in the illustration above. However, these stretches can provide some relief in the first instance of discomfort.
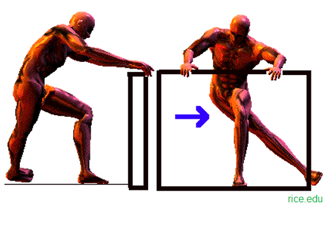
Regular sessions with a SRMT will keep the area maintained throughout the season and keep the fascia at the correct tension with various techniques.
By: Liz Ward








 When most people hear the word “Peloton” they think of an expensive black bike with shiny red buttons and that controversial commercial where the husband gifted his wife a Peloton for Christmas.
When most people hear the word “Peloton” they think of an expensive black bike with shiny red buttons and that controversial commercial where the husband gifted his wife a Peloton for Christmas. If the app interests you, Peloton is currently offering a 30 day FREE TRIAL, so why not give it a try? Check it out
If the app interests you, Peloton is currently offering a 30 day FREE TRIAL, so why not give it a try? Check it out 

 This article would not be complete, however, if we did not acknowledge some of the delivery issues that have been plaguing Peloton over the last year. Most of the delivery issues seem to affect U.S. deliveries, however, the UK deliveries have been affected as well.
This article would not be complete, however, if we did not acknowledge some of the delivery issues that have been plaguing Peloton over the last year. Most of the delivery issues seem to affect U.S. deliveries, however, the UK deliveries have been affected as well.







